Many people researching IVF and egg freezing ask about low-dose, minimal stimulation, and “natural” protocols (medication methods). Extend Fertility doesn’t routinely recommend mini IVF, because studies have shown that it’s significantly less effective and efficient. Keep reading to understand what mini IVF is, and how we approach IVF and egg freezing stimulation.
Want to learn more?
What are low-dose, mini, and natural IVF?
While these terms don’t have exact, industry-standardized definitions, they have general uses outlined below.
- Low-dose, minimal stimulation (“mini”), “mild” or “gentle” IVF is typically described as a cycle that uses lower doses of the injectable medications used in conventional IVF, or uses less powerful oral medications such as Clomid. A typical low-dose cycle may result in 1–4 eggs being matured and retrieved.
- Natural IVF is typically an IVF cycle that uses no medication whatsoever, but instead follows the natural ovulation cycle and retrieves the egg that’s naturally ovulated (if one matures). Natural IVF will result in a maximum of 1 egg retrieved, but may result in zero eggs.
Mini IVF has lower success rates
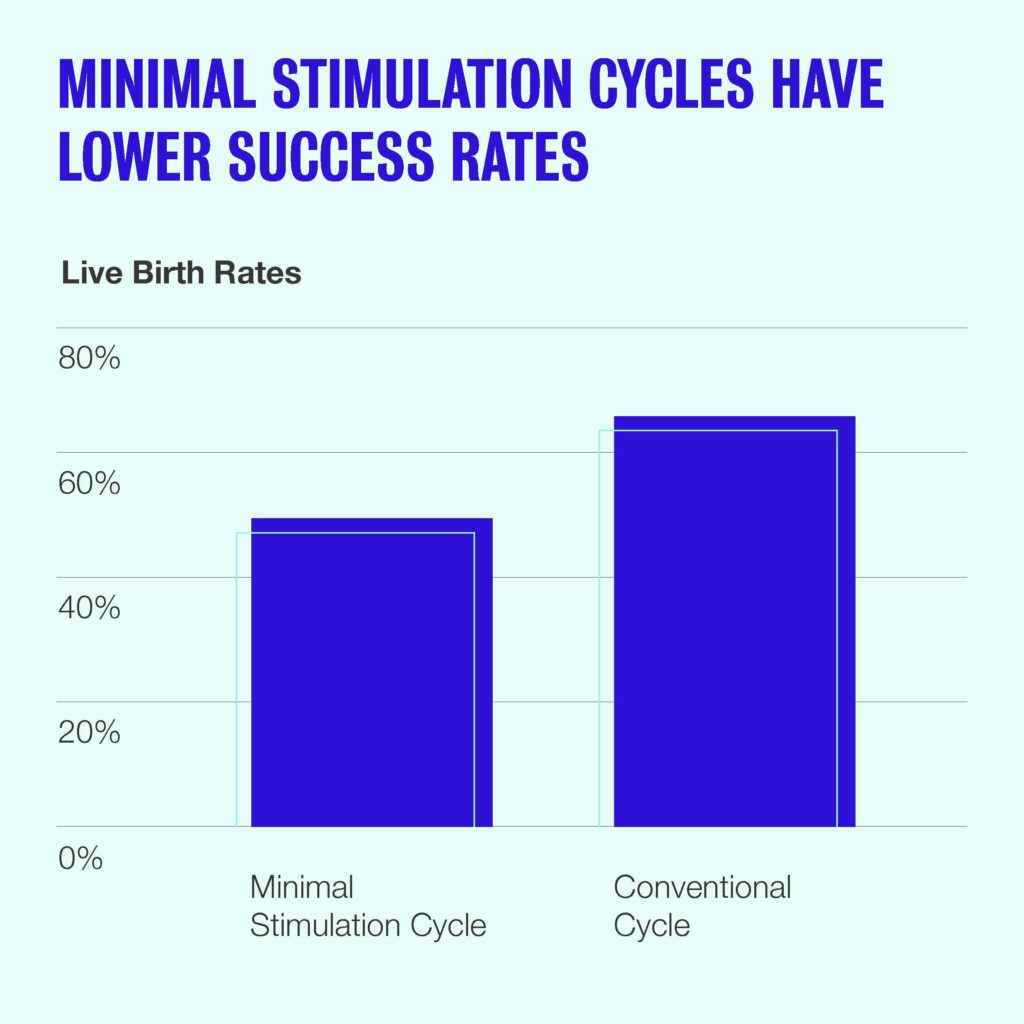
There’s an intuitively appealing idea that a more “natural” treatment is inherently better. But studies demonstrate that pregnancy rates are significantly lower after low-dose IVF cycles, and that the benefits of a “minimal” protocol don’t outweigh the cons. One study, published in the American Journal of Obstetrics and Gynecology in 2016, revealed that birth rates among minimal stimulation IVF patients were 49%, compared to 63% for conventional IVF patients.

This is because success rates are directly correlated with the number of eggs retrieved. Egg freezing and IVF is a “numbers game”; for patients of any age, a certain percentage of the eggs retrieved during an IVF or egg freezing cycle will be genetically abnormal (also known as “low quality”), and that percentage increases with age. So, the more eggs retrieved during a cycle, the higher the chances that a few of those eggs will be healthy and able to be fertilized.
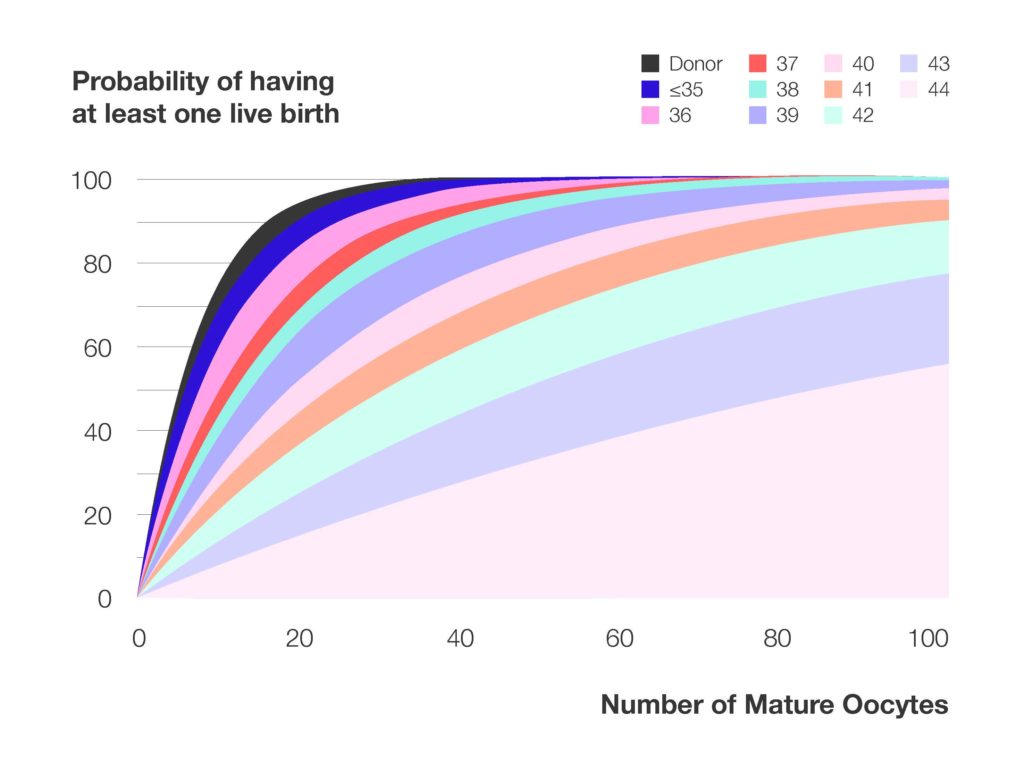
In a recent study of IVF success rates, live birth rates peaked for patients who retrieved 15 to 25 eggs. Studies of egg freezing success rates demonstrate a similar correlation; a model built by the team at Brigham & Women’s Hospital (results below) showed that success rates increased with the number of eggs frozen for patients of all ages.
There’s no evidence that mini IVF yields more high quality eggs
While many who promote natural and mini IVF protocols claim that lower doses of medication result in fewer, but higher quality eggs, there’s no evidence to support that idea.
For example, in the study of mini IVF mentioned above, birth rates were 22% lower for patients treated with minimal stimulation protocols. If it were true that low-dose IVF results in higher quality eggs, we would expect to see similar birth rates for cycles using minimal stimulation, if not higher.
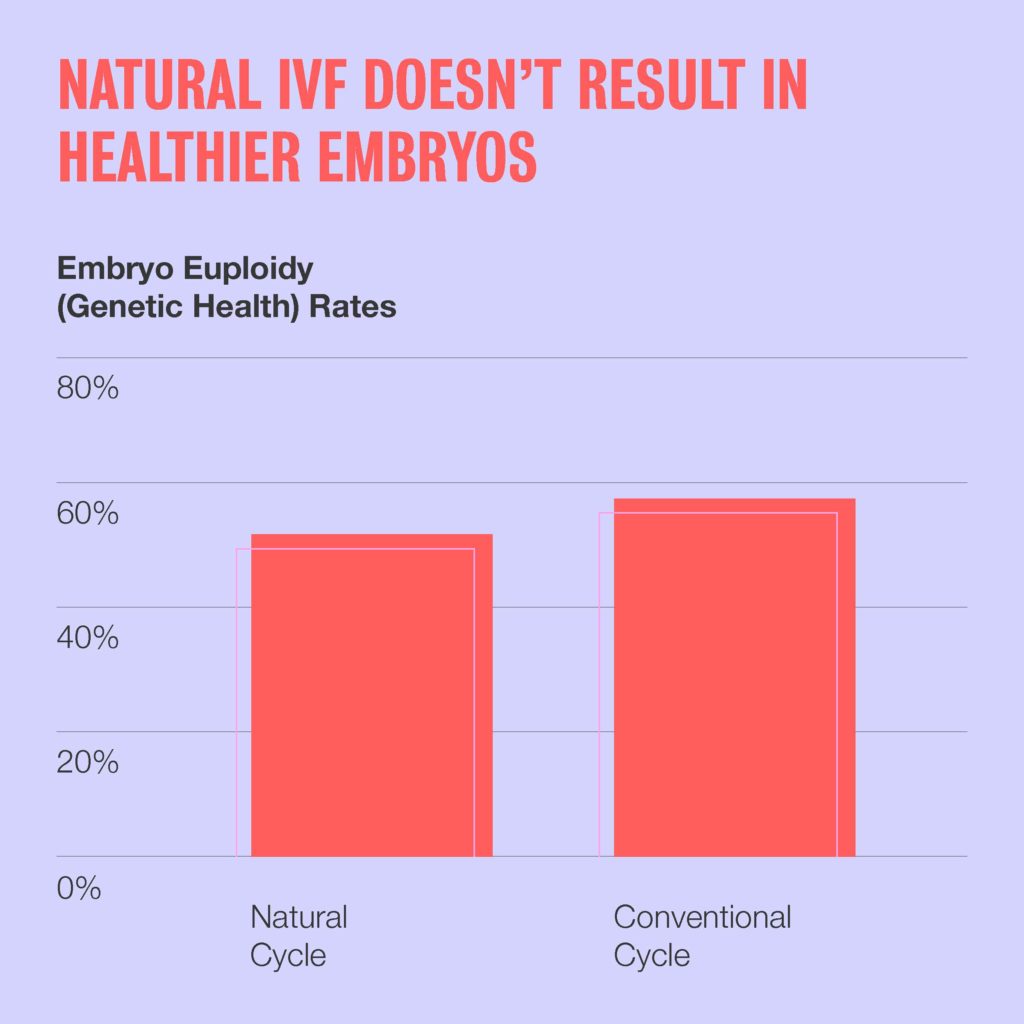
Another study of natural (unmedicated) IVF concludes similarly. In that study, 369 patients underwent natural IVF cycles and 1,845 patients underwent conventional IVF cycles; the embryos created were tested for genetic health. Researchers found that the ratio of normal and abnormal embryos was essentially the same in both types of cycles; there was no evidence that natural IVF improved egg quality. And, importantly, nearly a quarter of patients in this study using natural protocols went through their entire cycle without obtaining an egg; 78% of natural cycles didn’t have a single healthy embryo to transfer.
Mini IVF may not mean a lower cost
Because mini and natural IVF uses less, or no, medication, many patients believe it will be less expensive in the long run. That’s a logical idea, since medications are a big chunk of overall IVF and egg freezing costs ($3,000–$6,000 on average, if insurance doesn’t cover them). But because egg freezing and IVF success rates are so dependent on the number of eggs retrieved, what’s most likely is that the cost will simply shift from money spent at the pharmacy to money spent on additional cycles at your fertility clinic to obtain a healthy embryo or reach your egg freezing goal.
And then, there’s the additional emotional, social, and professional costs of multiple cycles: more days off from work, multiple retrieval procedures with anesthesia, and more weeks spent in the midst of an IVF or egg freezing cycle. These costs are more difficult to quantify, but should be considered when comparing the two protocols.
You can get the benefit of mini IVF with other modern IVF techniques
Mini IVF’s primary benefits is lower rates of ovarian hyperstimulation syndrome (OHSS), an uncommon overreaction of the ovaries to fertility medication that can cause fluid retention, bloating, and other symptoms. Because mini IVF uses lower doses of medication, it naturally has very low rates of OHSS.
However, with close monitoring and adjustment of medication doses, like we do here, the rate of severe OHSS is less than 1% of patients taking stimulation medications. Additionally, utilizing a Lupron trigger shot in place of an hCG trigger shot prior to the retrieval has been shown to nearly eliminate OHSS (here’s one such study), which is why we prescribe Lupron in most cases.
Our approach
Mini IVF doesn’t offer any singular benefits, and may significantly reduce pregnancy rates and increase the number of cycles required for success. But does that mean we use a cookie cutter method, prescribing the maximum dosage of medication for every patient? Absolutely not.
In addition to the close monitoring and use of Lupron trigger medication mentioned above, we improve outcomes and patient experiences by tailoring medications to a patient’s personal needs and goals. Prescribing medications is a balancing act: success rates with IVF and egg freezing are based on the number of eggs retrieved, but it’s also important to consider the patient’s overall egg “potential” and their experience throughout the egg freezing cycle.
For example, a woman undergoing IVF with a very low ovarian reserve will be expected to retrieve just a few eggs, and evidence tells us that giving her extra medication isn’t going to improve her outcome—but may increase her risk of negative side effects. In that case, we may use a lower dose protocol, because there’s no benefit to the patient to take more medications. We’ll tailor her dosage to get her the optimal result for herbody, as we do for each of our patients.
The bottom line: We believe in offering evidence-based treatment, and that’s why mini IVF is not a routine part of our practice. Want to learn more? Feel free to contact us to speak with a member of our healthcare team.