
Revolutionizing Fertility Care: A Breakthrough Study on Improving Access to and Outcomes of Fertility Treatments
Assisted reproductive technologies, such as IVF and egg freezing, provide promising solutions to the statistic that 1 in 6 individuals worldwide experience infertility and numerous others are interested in preserving their fertility. Currently, there is an issue with access to this care. Along with financial barriers, time constraints and medication side effects can prohibit those from receiving care. This is where we come in.
Addressing the Challenges of Fertility Care Access
One of the core pillars at Extend is accessibility to personalized and results-oriented care. And we are always looking to improve. This is why we teamed up with Gameto, a female-led biotech company developing treatment solutions to improve women’s reproductive health throughout their lives. In their latest study, the Gameto team set out to examine a new technology that allows for a reduction of time spent in a fertility treatment cycle (increasing access), using less medications (decreasing cost and side effects), while improving outcomes. Extend Fertility used their methods with consenting patients who donated their oocytes (eggs) to measure the effectiveness of this new method. Let’s dive into the study details and results!
The Study
S. Piechota, et al., Human-induced pluripotent stem cell-derived ovarian support cell co-culture improves oocyte maturation in vitro after abbreviated gonadotropin stimulation, Human Reproduction, 2023;, dead205, https://doi.org/10.1093/humrep/dead205
This study focused only on fertility treatments where individuals undergo a stimulation cycle to retrieve eggs. These retrieved eggs can be fertilized in a lab to create embryos and transferred into one’s uterus to achieve pregnancy. Currently, fertility clinics prescribe medication protocols to have eggs mature inside their ovaries at which point they are then retrieved. To reduce gonadotropin (the type of medication used in stimulation cycles) usage in fertility treatments, the application of minimal or abbreviated stimulation cycles is utilized. This in turn results in retrieving eggs that are immature. Since only mature eggs can be fertilized, immature eggs retrieved from abbreviated gonadotropin cycles can then undergo in vitro maturation (IVM) to mature eggs outside of the body. As the study states, numerous previous studies have employed IVM effectively, often through the application of reproductive cell culture media supplemented with growth factors, small molecules, and gonadotropins.* However, many of these studies have shown mixed results of IVM applications in terms of the rates of oocyte maturation, cleaved embryo formation, and blastocyst formation, with some studies showing lower pregnancy rates from IVM cycles. Therefore, improvement is needed in IVM strategies that yield robust, high-quality oocytes with strong developmental competence.
[Sidenote: The next line we are going to share might sound like a foreign language, however, we would like you to have the exact details of this revolutionary new technology!]
In this study, the researchers investigated the potential of hiPSC-derived OSCs (ovarian support cells) to improve IVM of oocytes in a co-culture system with immature cumulus–oocyte complexes (COCs) retrieved from subjects following abbreviated gonadotropin cycles.
Sidenote: By reading that, you basically just earned a new degree, congrats!
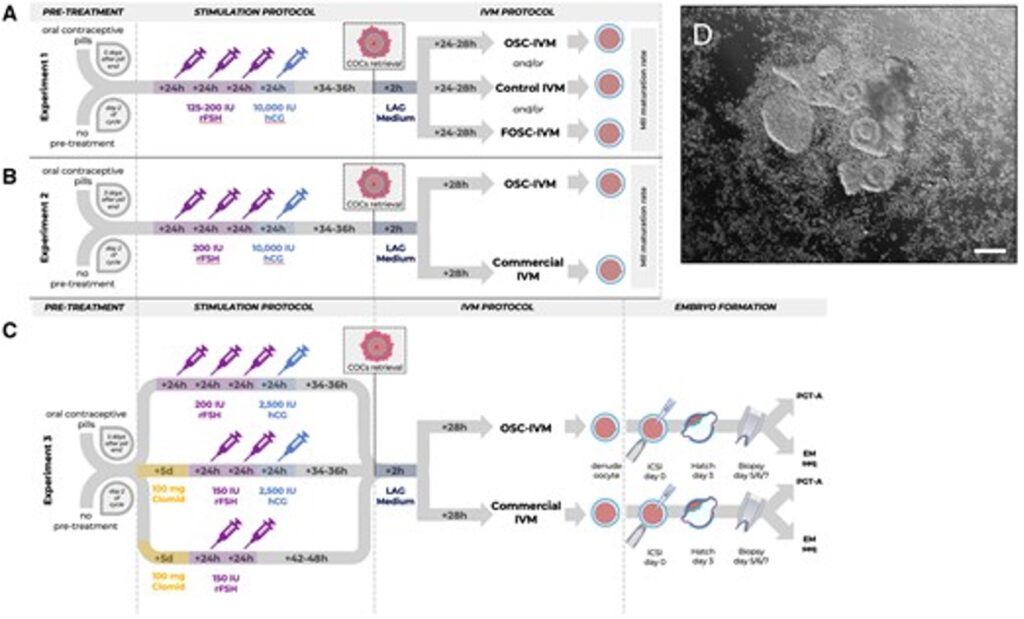
To save you from further medical terminology, this is a figure displaying the study design, which was broken out into three parts:
This is a figure that displays the study results – As you can see, OSCs (the method being tested) improve human oocyte maturation rates compared to supplemented IVM medium lacking OSCs or containing other cell types:
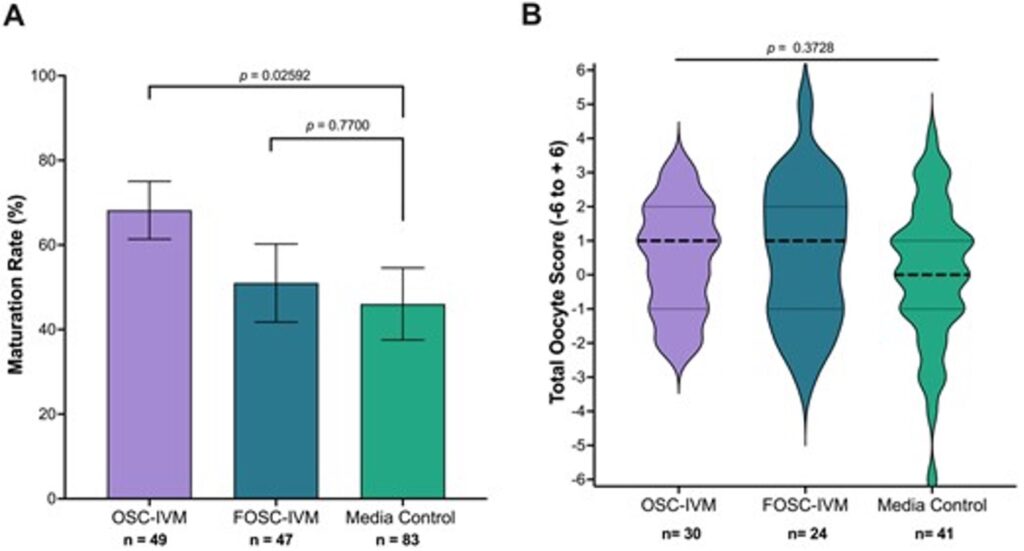
OSCs – The Game-Changer
As the first research study of its kind, the novel OSC-IVM approach resulted in the improvement of the rate and extent of egg maturation, yielding high quality eggs capable of healthy embryo formation. Additionally, this system outperformed media without OSCs and other cell lines as well as commercially available IVM culture media. Importantly, this study shows the value of applying this method in fertility treatments because eggs matured in the presence of OSCs have a high degree of developmental competence, meaning they can become healthy euploid embryos that would likely be competent to implant and become live born babies.
A Scalable and Cost Effective Solution
The best part? This method of IVM involving co-culture integrates readily with existing procedures employed in ART (Assisted Reproductive Technology) laboratories, requiring no special equipment and only minimal training for clinical embryologists. The OSC-IVM approach is generated from a single source of highly qualified, commercially available hiPSCs and does not require patient-specific generation. This approach would therefore be highly scalable, reproducible, and cost-effective as a novel IVM treatment for patients.
While this is very promising technology, the research is currently in its preliminary stages. Further validation and studies are needed before it can be applied in a clinical setting for our patients. The Extend Fertility team will remain committed to advancing technology in this field to achieve the best success rates possible for our patients.
*Sources: Shu-Chi et al., 2006; Fadini et al., 2009; De Vos et al., 2011; Moschini et al., 2011; Guzman et al., 2012; Pongsuthirak et al., 2015; Sánchez et al., 2017; Braam et al., 2019; Sanchez et al., 2019; Ma et al., 2020; Vuong et al., 2020a,b; Akin et al., 2021; Grynberg et al., 2022; Mohsenzadeh et al., 2022).




