There’s still a knowledge gap when it comes to fertility, studies say
According to a survey performed by Reproductive Medicine Associates of New Jersey in March, the gap between what people believe about their fertility and the actual biology is pretty wide.
The survey, which polled the beliefs of 1,000 adults between the ages of 18–40, demonstrated that 57% of respondents reported that they believed a woman’s “biological clock” stopped ticking at age 44. While it’s true that some women can have children naturally at age 44, fertility declines throughout a woman’s 20s and falls significantly after 35; only about half of women over 35 are able to achieve pregnancy in one year, compared with three-quarters of women under 31. By age 44, pregnancy rates are a mere 1–5%, with only about 2% of the remaining eggs deemed chromosomally normal. (Of course, the “biological clock” is an imperfect metaphor, but the fact remains that women have a very small chance of getting pregnant naturally over age 40.)
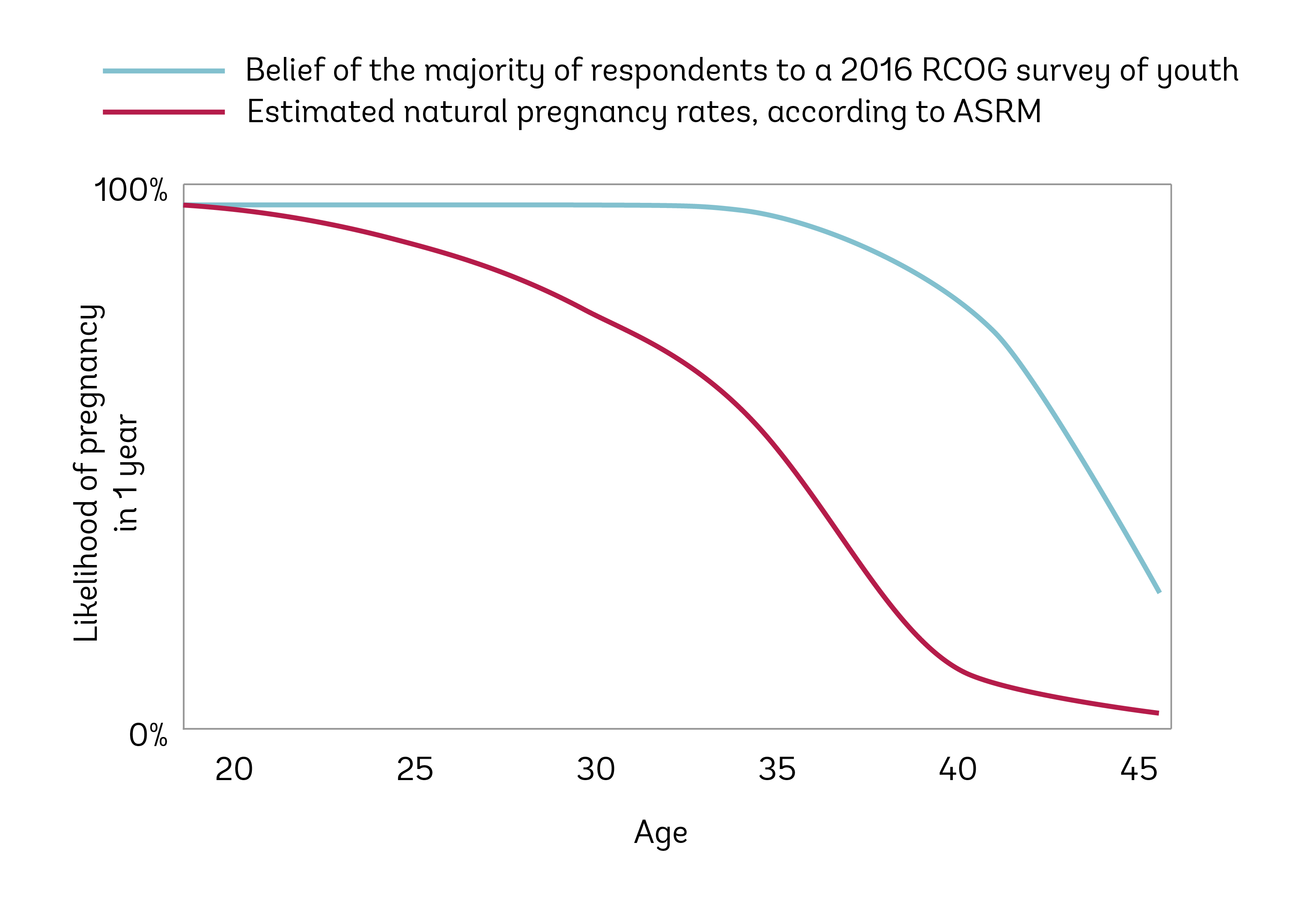
This survey is just the most recent in a series of studies examining public knowledge of fertility. Another recent survey performed by the Royal College of Obstetricians and Gynecologists in the UK examined the fertility perceptions of 1,000 young men and women between ages 16 and 24. A key takeaway from that survey? More than 80% of both sexes believe women’s fertility only begins to decline after age 35. (As we talk about often, fertility decreases throughout our adult lives—it’s just the more drastic decline that sets in at 35.) Additionally, a quarter of young men thought a woman’s fertility only starts to decline after the age of 40 (compared with 16% of girls). And yet another 2016 survey, this one by the Fertility Centers of Illinois, revealed that, of 1,208 American women ages 25–45 who had never been pregnant, only 48%—that’s less than half—understood that there was an age-related decline in fertility and increase in aneuploidy and pregnancy loss.
Contact Us to Chat with a Fertility Advisor
These recent results mirror those of the comprehensive 2011 study by pharmaceutical company EMD Serono that examined the fertility “IQ” of 1,010 women aged 25–35 who had never given birth and were not actively trying to conceive. Despite indicating that they plan to have their first child in their early to mid-30s, 73% of women in the Serono survey “anticipate that they would have an average, or easier than average, time conceiving than most women.” This belief doesn’t match reality: the survey reports remind us that 1 in 4 married women aged 35–44 experience infertility when attempting to have their first child, compared to only 1 in 10 of those under the age of 30.
Additionally, only a third of Serono’s respondents correctly identified age as the leading risk factor for infertility, and most believed that women over 40 have between a 10 and 40% chance of pregnancy in any given month—the actual monthly chance of pregnancy is only about 10%! The respondents also generally overestimated the success of IVF (believing IVF pregnancy rates to be 50–59% when they are actually 20–29%) and, importantly, were unaware of the importance of the age of the egg to in vitro fertilization success; 54% think that the chance of successful pregnancy via IVF does “not depend on the origin of the egg.”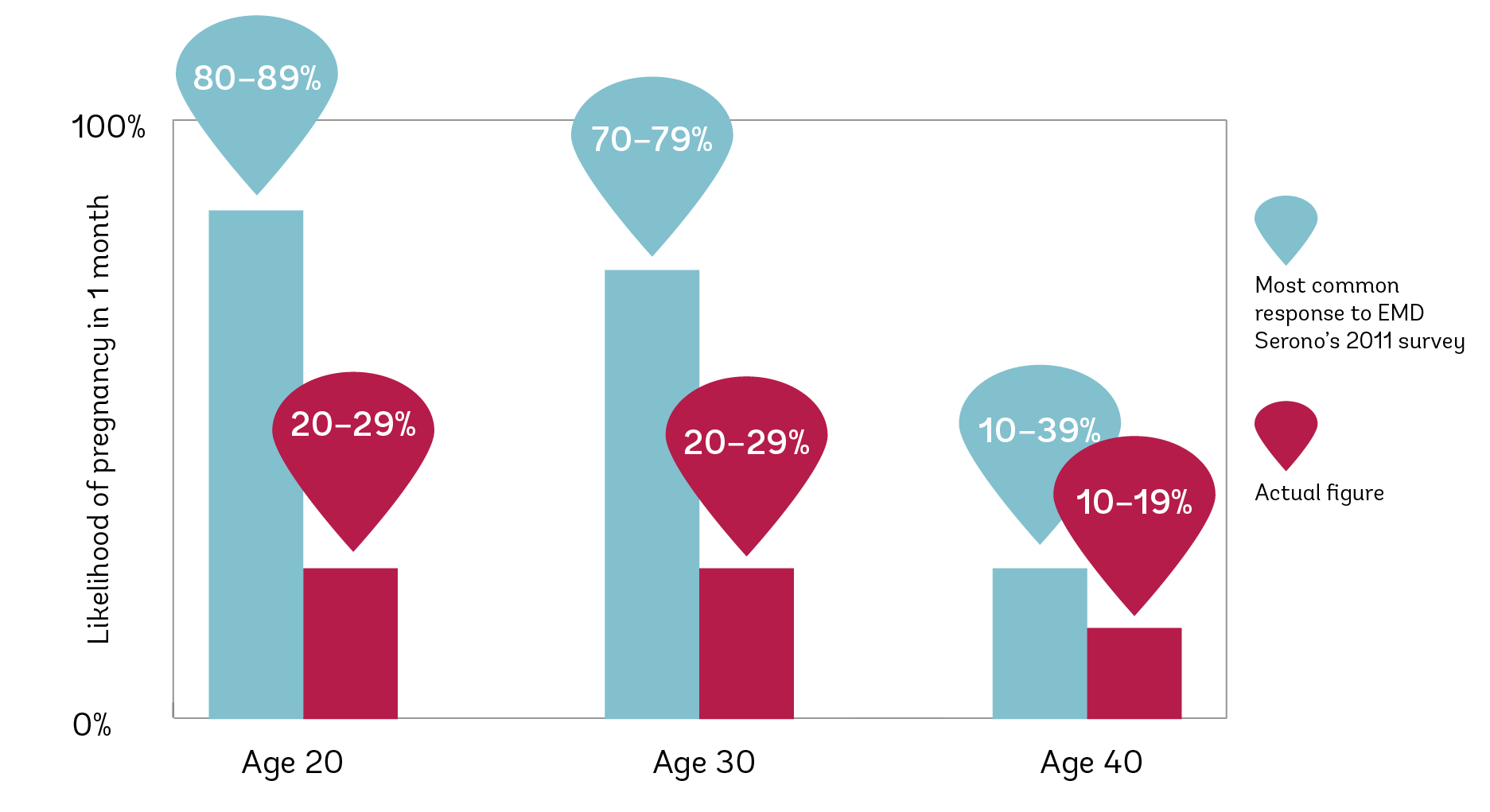
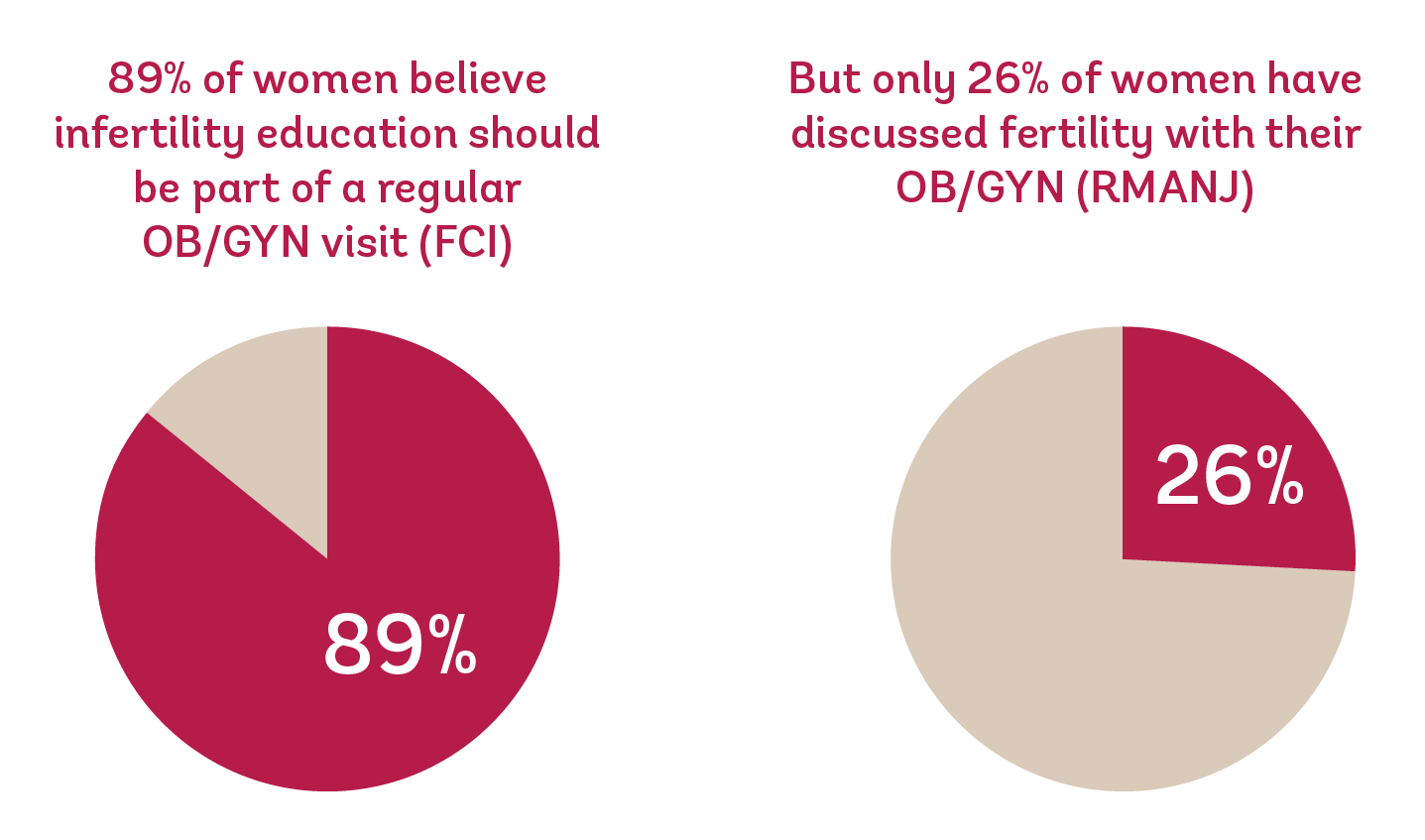
How can this be?! It seems like everywhere we look, people are talking about fertility—but it turns out they’re not having the conversation where and when it really matters. The RMANJ survey revealed that only 26% of women surveyed have had conversations with their OB/GYN about fertility and nearly half (42%) of women surveyed who had experienced infertility reported that their OB/GYN never started a conversation with them about fertility.
This again reflected the earlier EMD Serono survey results, which revealed that a majority of women never discussed future pregnancy plans (52%), age as an infertility risk factor (78%), or infertility treatment options (89–96%) with their OB/GYN. And it’s not because women don’t want this info; the Fertility Centers of Illinois reported that 89% of respondents agreed that infertility education should be mentioned at an OB/GYN visit and 52% of women age 35 or older stated that they would have made different life choices if they had known about the age-related decline in fertility.
Why aren’t women having this conversation with their doctors—before their fertility becomes a time-sensitive issue? Probably, it’s a combination of the fact that doctors aren’t always comfortable breaching the topic with patients (or there may not be time in an otherwise packed OB/GYN visit); the fact that there’s still a stigma surrounding fertility issues, childlessness, and fertility preservation; and the fact that women can’t ask their doctors about a problem if they’re not aware of it in the first place.
That’s why some experts are calling for fertility education at the high school level, and why Adam Balen, Chair of the British Fertility Society, is advocating for “choice, not chance,” saying, “Our aim is to ensure that sex and relationship education not only covers how to avoid pregnancies and sexually transmitted diseases, but also includes information about fertility and planning for the right time to start a family… We want to enable young people to make informed choices about pregnancy, whether that choice is to start a family or not.”
It’s also why we here at Extend Fertility are supporting OB/GYNs by providing them with the information they need to address the topic with their patients, and why we want to reduce the stigma around egg freezing, so more women feel comfortable talking to their doctors about it. And on that topic, the RMANJ survey brought us some good news: 80% of their respondents were in favor of fertility preservation. Hooray!




