New research suggests transgender men can have successful egg freezing treatment, even after testosterone therapy
Transgender men (assigned female at birth patients who identify as male or masculine) sometimes choose to undergo testosterone hormone therapy to align their secondary sexual characteristics, including facial/body hair, muscle mass and a deeper voice, with their gender identity.
Trans men can and do have healthy pregnancies. But, because little is known about the long-term impact of testosterone therapy on fertility, it’s often recommended that, if these patients would like to have genetic children in the future, they freeze their eggs prior to starting gender-affirming treatment. Egg freezing also gives transmasculine patients the option to use a gestational surrogate or do reciprocal IVF with a female partner in the future.
Learn more about egg freezing for transgender men.
A new study out of Boston IVF, published in late 2019, suggests that trans men who have undergone testosterone therapy have similar outcomes from egg retrieval cycles to cisgender women. This may mean that, even if you didn’t have the opportunity to freeze your eggs prior to starting gender-affirming treatment, you still have the option to preserve your fertility or start a family.
Study details
This study examined 8 years of patient data. It was fairly small, made up of 26 trans men patients along with a control group of 130 cisgender female patients of similar age and personal health. According to researchers, more than half of the trans patients had been taking testosterone therapy, and had paused that therapy for an average of 4 months before their ovarian stimulation cycle.
The ovarian stimulation process involves 8–11 days of hormone injections that prompt the ovaries to produce multiple eggs in one menstrual cycle, as opposed to the single egg typically produced. Then, those eggs are removed in a minimally invasive surgical procedure called the egg retrieval and either frozen immediately or fertilized to create embryos. More than half of the trans patients in this study (16 out of 26) were undergoing ovarian stimulation for egg freezing, while 7 were part of couples who did fresh or frozen embryo transfers.
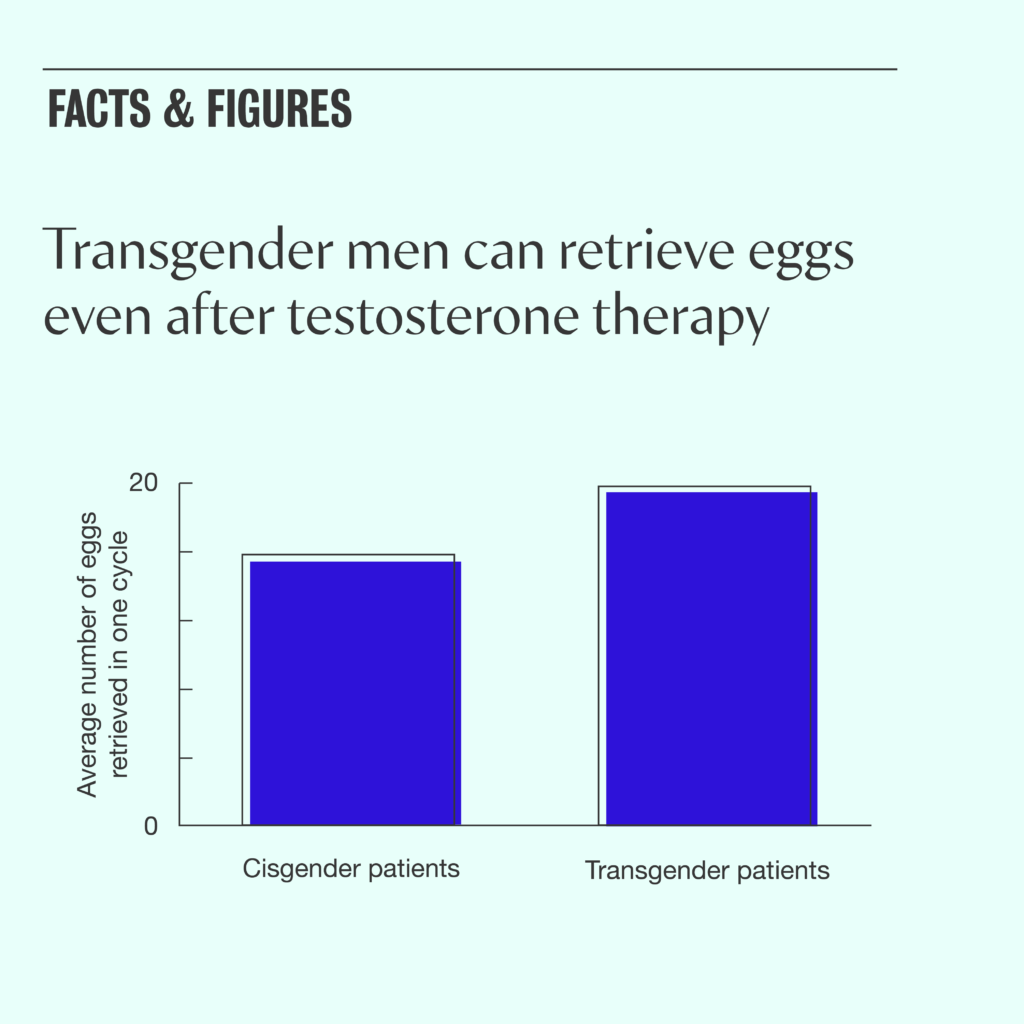
The average number of eggs retrieved in the transgender group was 19.9, compared to 15.9 in the cisgender group. Of the 7 couples who transferred embryos, all 7 achieved pregnancy and live birth.
Researchers have concluded that these results suggest that trans men who freeze their eggs have similar success rates to cisgender patients. As one of the researchers, Dr. Nina Resetkova, stated, the study found that “even long periods of gender-affirming androgen [testosterone] therapy did not appear to have a negative effect on ovarian stimulation outcomes.”
What else we need to know
While this study is ground-breaking, there’s still a lot we don’t know. We’ll need more, and larger, studies to confirm that testosterone therapy truly has no impact on fertility treatment outcomes; more research would also be helpful to understand whether the length of time that a patient has been taking gender-affirming hormone treatment changes that impact. Additionally, more research may illuminate whether or not testosterone treatment affects egg quality (health).
Finally, further studies will be necessary to understand how long trans men must stop taking testosterone before undergoing ovarian stimulation, and if it’s even necessary to stop testosterone therapy during fertility treatment.
Next steps: Learn more about egg freezing for transgender men or contact us to talk to a fertility advisor about your options.