Many people tend to think of fertility as something that pertains primarily to women, but in actuality, at least 30% of infertility cases can be attributed to male-factor infertility. This guide to male fertility testing will explain what the options are, when—and why—a man should test his fertility, and what happens if you don’t get the result you’re hoping for.
Learn more about male fertility decline and sperm health.
The cornerstone of male fertility testing: the semen analysis
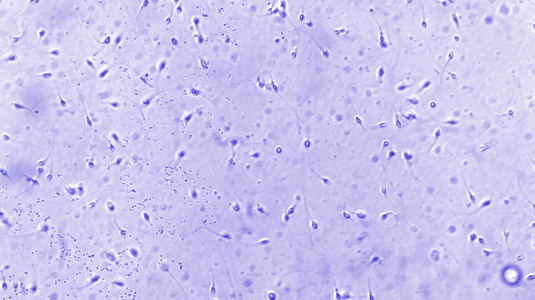
The first step in male fertility testing is the semen analysis. A semen analysis is a fairly simple, non-invasive test in which a semen sample, typically produced via masturbation, is examined under a high-powered microscope to determine the quantity and quality of sperm.
What a semen analysis tests for:
Sperm concentration (quantity)
Sperm concentration is the measure of how many sperm are present per milliliter of semen. Sperm concentration is found by calculating the number of sperm per milliliter of semen. A normal sperm concentration, according to the World Health Organization, is at least 15 million sperm per mL.
Why is sperm concentration important for male fertility? Because, after ejaculation, the sperm encounter many obstacles on their way to the egg: the acidity of the vagina, the cervical mucus (which can either help or hinder sperm’s journey toward the egg), and the possibility that they could get stuck somewhere else in the reproductive system—like up the wrong fallopian tube. Experts estimate that less than 1% of sperm actually make it to the egg, so it makes sense that it’s helpful to start with a lot.
Sperm motility (movement)
Sperm motility refers to how sperm move. Sperm are propelled forward by flagellations of their tail, plus a little help from the female reproductive system. The movement of sperm impacts whether or not they make it to the egg, and—once they do make it—whether they can penetrate the egg to fertilize it.
The ideal way for sperm to move is in straight lines or in large, sweeping circles. Motility is a measure of what percentage of sperm are moving, and progressive motility is a measure of what percentage of sperm are moving in this optimal way. According to the WHO, at least 40% motile sperm (with at least 32% moving progressively) is a normal result.
Fun fact: While it was believed for centuries that sperm moved forward thanks to quick back-and-forth movements of their tail (kind of like fish), a groundbreaking study published in July 2020 revealed that sperm actually “roll as they swim, much like playful otters corkscrewing through water.” This doesn’t change the importance, or the measurement, of motility, as the corkscrew motion can only be seen with super high-tech equipment—but it does give sperm a little more personality.
Sperm morphology (shape, size, and structure)
The proper sperm anatomy, according to male fertility company Legacy, looks like the following:
- a tail, which helps it “swim” toward the egg,
- a midpiece, containing mitochondria to power the sperm’s movement,
- a head, housing the nucleus (where genetic material for the potential offspring is stored), and
- an acrosomal vesicle, a structure at the tip of the sperm that contains enzymes to help the sperm penetrate the egg.
If a sperm is deformed—if it has multiple heads or tails, no head or tail, improperly formed sections, or it’s too big or too small—it may have difficulty moving toward the egg or fertilizing it. Morphology is the measure of what percentage of sperm have the proper shape, size, and structure, also known as “normal forms” (NF). According to the WHO, a normal morphology result is 4% NF or higher.

Semen factors
Semen volume refers to the amount of fluid that’s ejaculated. Typically, a low semen volume—less than 1.5mL according to the WHO—alone is not going to greatly impact male fertility, but it can indicate a blockage in one or more of the ducts/gland of the male reproductive system, and can compound the issue of low sperm count.
In addition to volume, male fertility testing may evaluate the pH level and chemistry of the semen. Again, abnormalities in semen pH or composition may point to a problem in the testicles, such as an obstruction or infection.
All four of the above “semen parameters” are important to consider when talking about male fertility testing.
In-office vs. at-home male fertility testing
A semen analysis is often performed in a fertility or urology office where there’s an andrology (male health-focused) laboratory. The process goes something like this: the male patient receives a sterile specimen cup for his semen sample. He can collect the sample, via masturbation, either in a “collection room” at the office, or produce it at home and bring it to the office, ideally within one hour.
The experience of producing or providing a semen sample at the office, while very common and nothing to be ashamed of, can be uncomfortable for many men. That’s why companies like Legacy offer at-home sperm testing kits that allow patients to collect their sample in the comfort of their own homes, combine the sample with special preservation media, and then mail it to the lab. This eliminates the need to go into the office at all, making it more convenient and less awkward.
A note of caution: many at-home male fertility testing products only test for sperm count, which—as we discussed above—is only part of the picture of male fertility. Make sure that, if you go this route for male fertility testing, the product you choose offers a comprehensive report on all sperm parameters.

As a Legacy partner, we’re offering a 10% discount on at-home semen analysis and sperm freezing kits to Extend Fertility patients and readers. Use the code extendlegacy at checkout!
Advanced male fertility testing
While semen analysis is the first step in male fertility testing, there are more advanced tests that can sometimes be used to diagnose less common conditions.
DNA fragmentation testing
As discussed above, the sperm carry genetic material—half of it, to be exact—for the potential future offspring. In a perfect scenario, this genetic material combines with the other half of the DNA, carried by the egg, to create a fully realized, unique embryo cell, which then divides as the embryo develops.
But, as with egg quality, the DNA sperm are carrying can be damaged, making it harder for that sperm to properly fertilize an egg and create a healthy baby. This is known as DNA fragmentation, and it’s associated with lower pregnancy rates and higher rates of abnormal embryos. While advanced paternal age is associated with DNA fragmentation, other common causes include infection or illness with high fever, cigarette smoking or drug use, and toxin exposure.
There are several options for male fertility testing for DNA fragmentation. The most common tests include the sperm chromatin structure assay (SCSA); the deoxynucleotidyl transferase-mediated dUTP nick end labeling assay (TUNEL), the single-cell gel electrophoresis assay (COMET), and the sperm chromatin dispersion test (SCD). (Hooray for acronyms!) While the technology used by each of these tests is slightly different, the goal is the same: to assess the general state of the DNA within sperm.
Sperm DNA testing is not standard male fertility testing, and because these tests only look at a portion of the millions of sperm in one semen sample, they may not accurately represent the genetic health of the entire sample. But this type of testing is an option for men who have specific, known risk factors for sperm DNA fragmentation.
Antisperm antibody testing
Rarely, fertility may be impacted by “antisperm antibodies,” proteins from the immune system that mistakenly attack and destroy sperm. ASAs may be found in semen or even directly bound to sperm. ASAs are not a normal product of the body’s immune response—they’re typically developed as a result of some form of trauma to the male reproductive system, such as testicular torsion, biopsy, or vasectomy.
Because the presence of ASAs are rare, they’re also not a routine part of male fertility testing. A doctor may order a test to identify ASAs in semen if a man has a normal sperm concentration, but very low sperm motility (a condition known as asthenospermia).
Why to do male fertility testing
Obviously, the most common reason to do male fertility testing is because a couple is trying to conceive, or may be having difficult getting or staying pregnant. But you may also do a semen analysis before freezing your sperm (to freeze the healthiest possible sample), after a vasectomy (to ensure it’s worked) or vasectomy reversal (to ensure sperm parameters are recovering properly), or just to have additional data points about your overall health.
When to do male fertility testing
Historically, doctors have recommended fertility work-ups after 12 months of trying to conceive (or 6 months, if the female partner is over 35). However, experts like those at Legacy contend that performing basic male fertility testing, such as a semen analysis, earlier in the process of trying to get pregnant may be beneficial.
Why? First of all, semen analysis is non-invasive and not unreasonably expensive (in-office testing is around $250, while Legacy’s at-home kit costs $150). And secondly, because men can improve their fertility with lifestyle changes (more on that below), testing the male partner’s fertility early on and taking steps to improve it may save time and money in the long run.
Next steps after male fertility testing
So, you’ve done a semen analysis—what’s next? That depends on your results. If everything is normal, you might consider freezing your sperm. If you’re having difficulty conceiving and a semen analysis didn’t reveal anything notable, you might next consider meeting with a reproductive endocrinologist to discuss female fertility screening or treatment options (if you haven’t already).
But if your results weren’t optimal, you do have some options:
Improving male fertility
Unlike eggs, which are in the ovaries since before birth and aren’t really impacted by most of the lifestyle choices women make, sperm are created every day, and their health can be significantly affected by diet, exercise, smoking, drinking, and even sleep, among other factors. Some men will find that, simply by improving their lifestyle habits—quitting smoking, starting an exercise regimen, or including more veggies and healthy fats in their diet—they can improve their sperm on their own, without medical intervention. (We recommend Legacy’s sperm improvement guide as a great place to start.)
Spermatogenesis, the process of creating sperm, takes about 74 days, so if you do implement changes, expect that it will be 2–3 months before you see a difference in your fertility. You may also want to repeat male fertility testing 2–3 months after making a lifestyle change, to assess how well it worked.
Treatment options for male infertility
If you’ve made lifestyle changes but are still having difficulty conceiving, there are treatment options to address male-factor infertility.
IUI
IUI or intrauterine insemination is a process in which a semen sample is washed (AKA, healthy sperm are isolated from the rest of the seminal fluid) and then inserted directly into the uterus, bypassing the vagina and the cervix. Because IUI gives sperm a “head start”—and because it’s done precisely at the time of ovulation—it can boost chances of pregnancy for those with mild male-factor infertility. Learn more about IUI.
IVF with ICSI
In vitro fertilization (IVF) is a more powerful fertility treatment, and paired with intracytoplasmic sperm injection (ICSI) can treat even the most severe cases of male-factor infertility. During IVF, the female patient’s ovaries are stimulated with medication to create several eggs; those eggs are then removed from the ovaries in a surgical procedure and brought to the lab. In the lab, an embryologist can perform ICSI, the process in which a single sperm is injected directly into an egg to aid fertilization.
Because ICSI requires only one sperm per egg, and can facilitate fertilization even when sperm are morphologically abnormal or not progressively motile, it’s the most effective treatment for many male fertility issues.
Sperm extraction
In some cases, sperm may not be developing properly, or may not proceed as they should from the testicles into the semen (possibly due to issues with spermatogenesis, congenital absence of the vas deferens, severe ejaculatory dysfunction, or other diagnoses). An option for these men is sperm extraction or aspiration directly from the testicular tissue. There are a few different procedures that can accomplish this goal: testicular sperm aspiration (TESA), which a small sample of testicular tissue is removed and examined for the presence of sperm; testicular sperm extraction (TESE), in which the testicle is surgically opened to allow for a larger sample to be taken; or percutaneous epididymal sperm aspiration (PESA), in which a needle is used to take fluid from a duct behind the testes, which will then be examined for sperm.
Because sperm extraction or aspiration typically results in few, lower-quality sperm, it’s used in conjunction with IVF and ICSI.
Medication
Depending on the diagnosis, a doctor may be able to treat male infertility with oral or injectable medication. According to Legacy’s sperm improvement guide, three of the most common medications are:
- clomiphene citrate (or “Clomid”), an estrogen-blocking medication that can increase levels of testosterone, luteinizing hormone, and follicle-stimulating hormone to improve sperm count/concentration and motility;
- anastrozole, a medication that also decreases estrogen levels and increases levels of testosterone, FSH, and LH to support sperm production; and
- human chorionic-gonadotropin (hCG) and human menopausal gonadotropin (hMG), which can be used to treat hormone imbalances in testosterone and LH that lead to low sperm count and other fertility issues.
Still have questions about male fertility testing? Learn more about male fertility decline and sperm health—or contact us to schedule an infertility consultation with our team.