The first step is to schedule a fertility assessment, during which our healthcare team will gather information for your consultation with one of our accomplished reproductive endocrinologists. You’ll also meet your fertility advisor, who will guide you through each step of the process.
What to bring:
Recent blood test and Pap smear results
If you’ve had any hormone, HIV, or STI blood tests completed in the last 12 months, bring the results with you—it might be one fewer test we’ll have to run after your first visit. Bring Pap smear results completed in the last 12 months, too.
Any relevant medical records
If you have any significant medical history that might come up in your conversation with the doctor—like a history of gynecological issues, surgeries, or long-term medical treatment—bringing medical records can be helpful.
The date of your last menstrual period
If your period is regular, this will help the team understand where you are in your cycle.
What to expect:
Meet your fertility advisor
As you move forward, your fertility advisor will stick with you through the whole process to make sure you always have the answers and support you need.
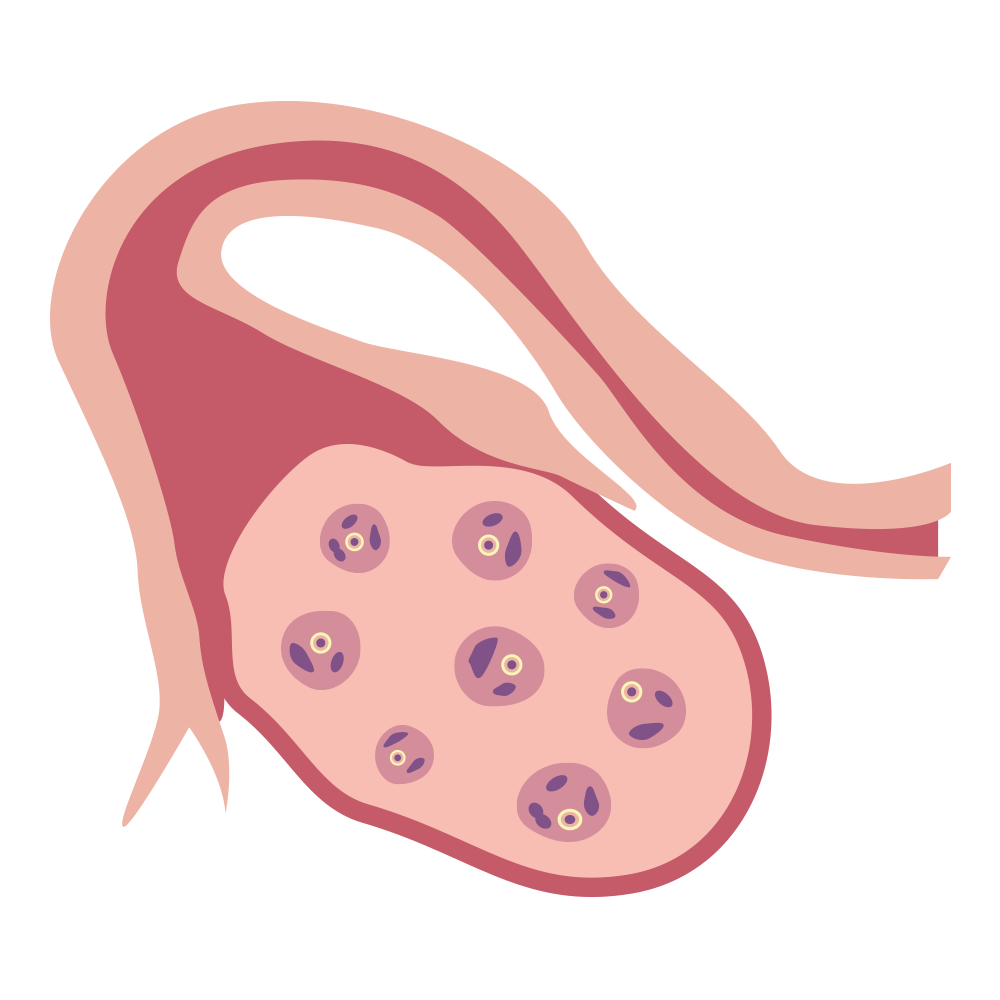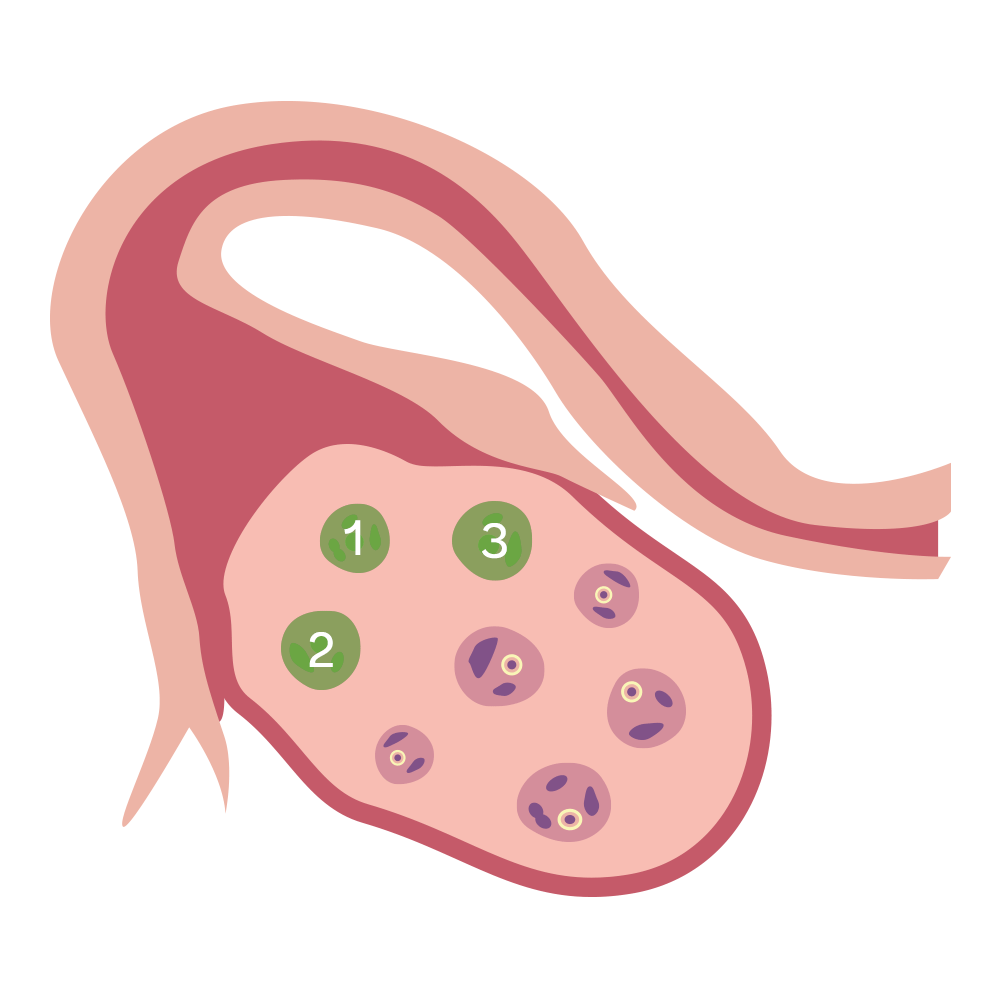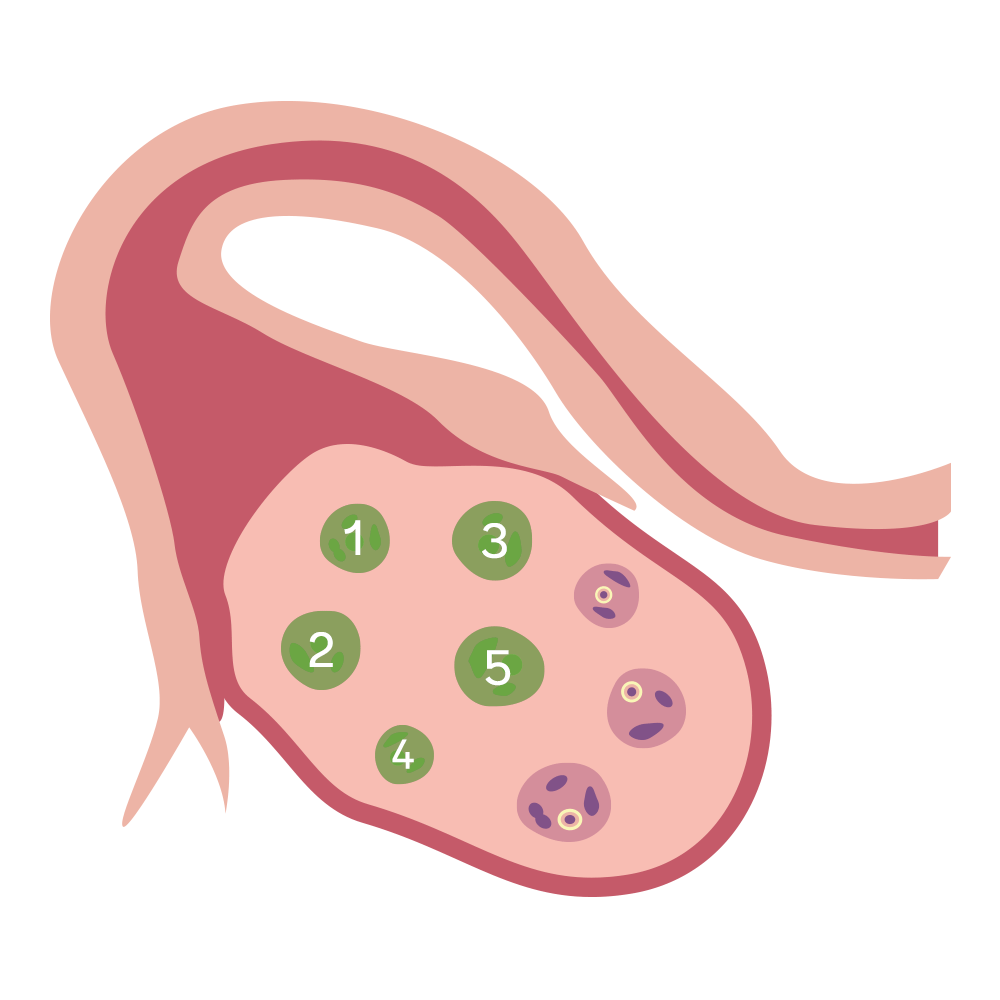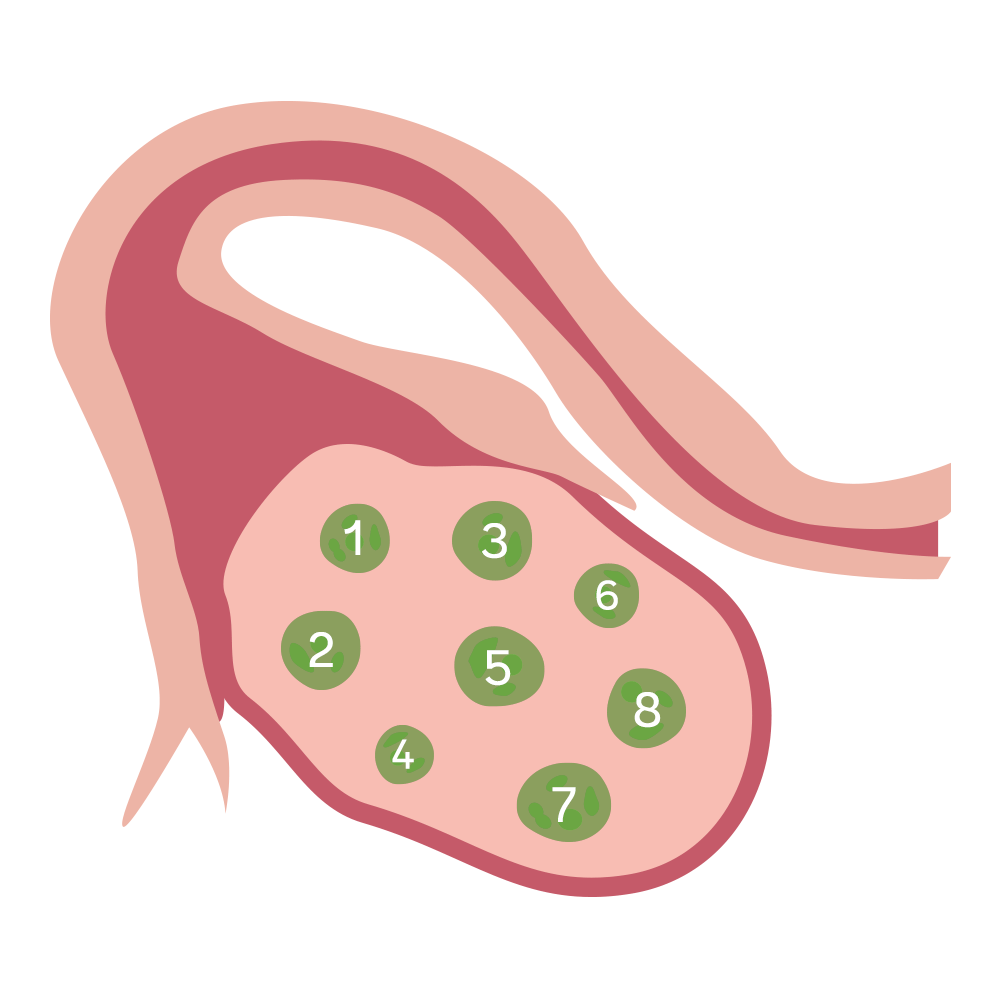
A transvaginal ultrasound
We’re born with all the eggs we’ll ever have, and with each passing month we either use ‘em or let ‘em go. So the older we get, the fewer we have in our reserves (literally—it’s called your “ovarian reserve”). One of the best ways to estimate your egg quantity is a transvaginal ultrasound. During a transvaginal ultrasound, a doctor places an ultrasound wand into your vagina in order to get a picture of your uterus and ovaries. It usually doesn’t hurt, but it can be a bit uncomfortable, like a gynecological exam.
This ultrasound allows the doctor to count the number of egg follicles, or the structures that hold individual eggs, in your ovaries. This number is called your antral follicle count. Generally, the higher the antral follicle count, the higher the ovarian reserve.
Blood testing
The other way to estimate your ovarian reserve is through a blood test that measures your AMH, or Anti-Müllerian Hormone.
AMH is a protein hormone produced by special cells inside the follicles. The level of AMH in the blood can help doctors estimate the total number of follicles inside the ovaries, and therefore a woman’s total egg count. A typical AMH level for a fertile woman is 1.0–4.0 ng/ml, but, depending on age, many women will be higher or lower than this range.
What comes next:
A consultation with one of our reproductive endocrinologists
Once the healthcare team has gathered all the necessary information, you’re ready to schedule a consultation with one of our reproductive endocrinologists (physicians who specialize in fertility). At this meeting, you’ll discuss your fertility, your age, and your medical history, as well as your goals for the future.
You’ll also talk about the egg freezing process. Knowledge is power, so you should expect to be fully informed throughout every step of freezing your eggs. Your physician will explain everything, including the medication, the egg retrieval procedure, and cryopreservation, at this first meeting.
Your chance to ask questions—seriously, anything goes!
We understand you might have a lot of questions at this point. That’s a good thing! This is your time, so feel free to bring a list of questions to your consultation so you don’t forget anything. We want you to have all the information you need to feel comfortable with whatever decision you make about egg freezing. (Don’t freak out if you do forget something during the consultation—the physicians and staff are here to answer all your questions throughout the process.)
Please note that we offer physician consultations to you at no cost, but we do ask for 48 hours’ notice if you need to cancel or reschedule. This allows us to make these very valuable appointments available to other patients. If you cancel or reschedule without 48 hours’ notice, we will apply a $50 cancellation charge to your credit card.
We won’t be charging you a fee for the fertility assessment or the consultation—or any fees at all, until you decide to freeze.
Get the FAQs
You probably have questions—we’ve got you covered with our comprehensive FAQs, organized by topic. Something you don’t see? Just ask!

